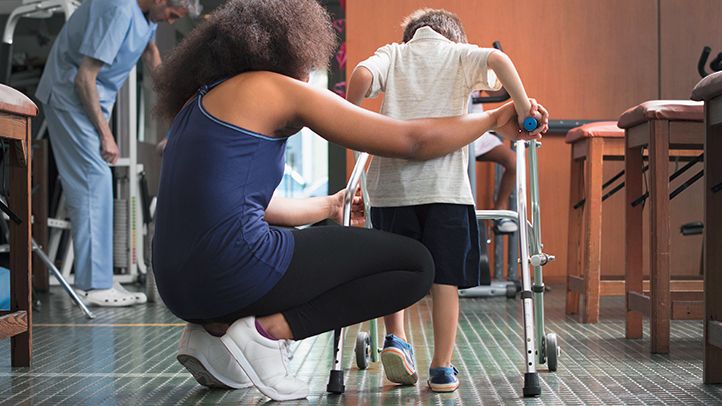Duchenne muscular dystrophy (DMD) is a genetic disorder characterized by progressive muscle degeneration and weakness. Physical therapy plays a crucial role in managing DMD by focusing on maintaining range of motion, preventing contractures, promoting mobility, and improving strength through targeted exercises. It can also help with respiratory management and functional abilities. However, it’s important for physical therapy to be tailored to each individual’s needs and stage of the disease progression.
What is Duchenne muscular dystrophy?
Duchenne Muscular Dystrophy (DMD):
Duchenne Muscular Dystrophy is a rare genetic disorder characterized by the progressive degeneration of muscle tissue. It primarily affects young boys, with symptoms often appearing between the ages of 3 and 5. DMD is caused by a mutation in the DMD gene, which leads to the absence of a vital muscle protein called dystrophin. This deficiency results in muscle weakness and eventual loss of mobility.
Relevant anatomy:
Duchenne muscular dystrophy (DMD) is a genetic disorder that primarily affects muscle tissue. The related anatomy includes:
- Muscles: DMD primarily impacts skeletal muscles, which are responsible for voluntary movements like walking and lifting objects. Over time, these muscles weaken and deteriorate.
- Dystrophin: The absence or dysfunction of the dystrophin protein is a hallmark of DMD. Dystrophin is crucial for maintaining muscle cell integrity and stability.
- Muscle Fiber: Muscle fibers are the building blocks of muscles. In DMD, muscle fibers undergo damage and degeneration, leading to muscle weakness and atrophy.
- Connective Tissue: Surrounding muscle fibers, there’s connective tissue called fascia. It plays a role in muscle support and protection.
- Nervous System: The nervous system controls muscle movements. DMD doesn’t directly affect the nervous system but impairs muscle function, leading to mobility issues.
- Heart Muscle: DMD can also affect the heart muscle (cardiac muscle), leading to cardiomyopathy and heart problems.
- Bones and Joints: Weak muscles can lead to joint contractures and bone deformities as a result of reduced mobility.
- Respiratory Muscles: DMD can impact the muscles needed for breathing, which can lead to respiratory complications as the disease progresses.
Causes:
Duchenne muscular dystrophy (DMD) is primarily caused by mutations in the DMD gene. These mutations result in the absence or dysfunction of a protein called dystrophin, which is crucial for muscle cell stability. The main causes include:
- Genetic Mutation: DMD is an inherited genetic disorder caused by mutations in the DMD gene located on the X chromosome.
- X-Linked Recessive Inheritance: DMD primarily affects males because they have only one X chromosome. Females typically carry the mutation as carriers but are often asymptomatic.
- Deletion or Frame-Shift Mutations: Most DMD cases involve large deletions or frame-shift mutations in the DMD gene, leading to non-functional dystrophin protein.
- Lack of Dystrophin: Dystrophin is essential for muscle cell integrity, and its absence or dysfunction causes progressive muscle degeneration.
- Muscle Weakness and Wasting: Without functional dystrophin, muscle fibers weaken, break down, and are replaced by fatty and connective tissue, causing muscle weakness and wasting.
- Progressive Nature: DMD is progressive, leading to loss of mobility and life-threatening complications due to respiratory and cardiac muscle involvement.
- Sporadic Mutations: In some cases, DMD can occur due to spontaneous mutations, not inherited from parents.
Symptoms:
Here are some common symptoms of Duchenne muscular dystrophy:
- Progressive muscle weakness, typically starting in the legs and pelvis.
- Frequent falls and difficulty getting up from a seated or lying position.
- Delayed motor milestones, such as walking later than usual.
- Waddling gait and difficulty running.
- Muscle stiffness and contractures (tightening of muscles and tendons).
- Difficulty with fine motor skills, like writing or buttoning clothes.
- Enlarged calf muscles (due to muscle fiber replacement with fatty tissue).
- Cardiac issues, as the heart muscle weakens over time.
- Respiratory problems, including difficulty breathing and reduced lung function.
- Cognitive and behavioural challenges, though these are less common and variable.
How to diagnose the Duchene muscular dystrophy?
Early Signs and Diagnosis
Identifying DMD in its early stages is crucial for intervention. Parents and caregivers should be vigilant for signs such as difficulty walking, frequent falls, and delayed motor skills development. A definitive diagnosis is typically made through genetic testing and muscle biopsy.
The diagnosis of Duchenne muscular dystrophy typically involves several steps:
- Clinical Evaluation: A doctor will begin by taking a detailed medical history and performing a physical examination. They will look for signs of muscle weakness, delayed motor milestones, and other characteristic symptoms.
- Blood Tests: Blood tests may be conducted to check for elevated levels of creatine kinase (CK), which is often elevated in individuals with DMD due to muscle damage.
- Genetic Testing: The gold standard for diagnosis is genetic testing, usually through a blood sample. This can identify mutations in the DMD gene responsible for the condition. Techniques such as DNA sequencing and deletion/duplication analysis are commonly used.
- Muscle Biopsy (if needed): In some cases, a small sample of muscle tissue may be taken through a biopsy to confirm the presence of muscle degeneration and to rule out other muscle disorders.
- Electromyography (EMG): EMG measures the electrical activity in muscles and can help differentiate between DMD and other neuromuscular disorders.
- Imaging: Techniques like MRI (Magnetic Resonance Imaging) or ultrasound may be used to visualize muscle tissue and assess its condition.
- Family History: A family history of DMD or related muscular dystrophies can be an important factor in the diagnosis.
What are treatment options for Duchene muscular dystrophy?
Current Treatment Options:
While there is no cure for DMD, various therapies and treatments aim to manage the condition and improve the quality of life for those affected:
- Physical Therapy:
Physical therapy plays a central role in the management of Duchenne Muscular Dystrophy. It focuses on maintaining muscle function, preventing contractures, and optimizing mobility. Therapists work with patients to create tailored exercise plans that target specific muscle groups.
- Corticosteroids:
Corticosteroids, such as prednisone and deflazacort, are commonly prescribed to slow down muscle degeneration and maintain muscle strength. These medications can help delay the progression of the disease.
- Assistive Devices:
As the condition progresses, individuals with DMD may require assistive devices such as braces, wheelchairs, or mobility aids to enhance their independence and mobility.
- Emerging Therapies:
The search for more effective treatments for DMD is ongoing. Promising approaches include gene therapy, exon skipping, and stem cell therapy. These cutting-edge treatments offer hope for slowing down the disease’s progression and improving the overall quality of life for those affected.
- Coping and Support:
Living with Duchenne Muscular Dystrophy can be challenging, both for patients and their families. It is essential to establish a strong support network, access specialized care, and stay informed about the latest advancements in DMD research and treatment options.
What kind of role physical therapy play in the management of Duchene muscular dystrophy?
DMD Physical Therapy
Physical therapy can help individuals with Duchenne muscular dystrophy (DMD) in several ways:
- Maintaining Muscle Function: Physical therapists design exercise programs to help preserve muscle strength and function, delaying the progression of muscle degeneration.
- Range of Motion: They work on maintaining or improving joint flexibility, preventing contractures (permanent muscle and joint tightness).
- Respiratory Support: DMD can affect respiratory muscles. Physical therapists teach breathing exercises to improve lung capacity and prevent respiratory complications.
- Mobility: Assistive devices like braces or wheelchairs may be needed. Physical therapists provide training in using these devices safely and effectively.
- Balance and Coordination: DMD can impact balance and coordination. Therapists work on these skills to enhance mobility and prevent falls.
- Pain Management: They employ techniques like massage, stretching, and modalities such as heat or ice to manage pain and discomfort associated with DMD.
- Adaptive Strategies: Physical therapists help patients adapt to daily tasks, making them more manageable and less physically demanding.
- Education: They educate patients and their families on managing symptoms, including the importance of staying active within the individual’s capabilities.
- Functional Independence: The goal is to maximize independence and quality of life, ensuring that individuals with DMD can perform daily activities as long as possible.
- Monitoring Progress: Regular physical therapy sessions allow therapists to assess the progression of DMD and adjust treatment plans accordingly.
What is a rehabilitation plan for Duchene muscular dystrophy?
Treatment plan:
A physical therapy treatment plan for Duchenne muscular dystrophy typically focuses on maintaining and improving mobility, muscle strength, and function while managing symptoms. Here’s a general outline of such a plan:
Initial Assessment:
- Comprehensive evaluation of the patient’s current physical condition, muscle strength, joint range of motion, and functional abilities.
- Assessment of any specific muscle weaknesses or contractures.
Individualized Exercise Program:
- Tailored exercise regimen to address specific weaknesses and maintain overall strength.
- Low-resistance exercises, such as swimming, stationary cycling, or gentle resistance training.
- Emphasis on regular stretching to prevent contractures and maintain joint flexibility.
Assistive Devices and Mobility Aids:
- Recommendation and training in the use of mobility aids like wheelchairs, braces, or orthotics, as the condition progresses.
- Ensuring proper fit and function of these devices.
Breathing and Respiratory Exercises:
- Techniques to improve respiratory muscle strength and function.
- Use of incentive spirometry or other devices to promote deep breathing and lung expansion.
Pain Management:
- Strategies to address pain and discomfort, which may include massage, heat/cold therapy, or positioning.
- Medication management under the guidance of a healthcare provider.
Education and Lifestyle Modifications:
- Educating the patient and their family about the condition, its progression, and symptom management.
- Teaching energy conservation techniques to optimize daily activities.
Adaptive Activities:
- Recommending adaptive recreational activities that promote social engagement and physical activity.
- Encouraging participation in activities appropriate to the patient’s abilities and interests.
Regular Monitoring:
- Periodic re-assessment of the patient’s condition and adjustment of the treatment plan as needed.
- Close collaboration with a multidisciplinary team of healthcare professionals, including physicians, occupational therapists, and nutritionists.
What are best exercises for Duchene muscular dystrophy?
Exercises:
Duchenne muscular dystrophy (DMD) is a progressive genetic disorder that affects muscle strength and function. Exercise should be approached with caution, and it’s essential to consult with a healthcare professional or physical therapist who is familiar with DMD to develop a safe and personalized exercise plan. Exercises may include:
Range of motion exercises:
Duchenne muscular dystrophy (DMD) can cause tightness in muscles and joints, limiting movement. Range of motion exercises are crucial to maintain flexibility and independence for as long as possible.
Examples of exercises:
- Ankle circles: Make small circles with your feet, both clockwise and counter-clockwise.
- Hamstring stretch: Lie on your back and bring one knee to your chest, gently pulling the hamstring with a strap or towel.
- Quad stretch: While standing, hold onto something for support and pull your foot up behind you to stretch the quadriceps muscle.
- Chest stretch: Stand in a doorway and place your forearms on either side of the frame. Gently lean forward to stretch your chest muscles.
Breathing exercises:
To maintain respiratory function and improve lung capacity. While there isn’t a one-size-fits-all recommendation for breathing exercises with Duchenne muscular dystrophy (DMD), some techniques can be helpful. It’s important to consult with a healthcare professional before starting any new exercises, especially for those with DMD.
Here’s some general information:
- Focus on lung expansion: Techniques like pursed-lip breathing and diaphragmatic breathing can help expand the lungs and improve oxygen intake.
- Maintaining airway clearance: Postural drainage and chest percussion might be recommended by a physiotherapist to help clear mucus from the airways.
- Yoga for lung function: Studies suggest yoga breathing exercises may improve lung function in DMD patients.
Hydrotherapy:
Hydrotherapy, also known as aquatic therapy, is a form of exercise that involves performing specific exercises in a warm-water pool under the supervision of a physiotherapist. It has been shown to be beneficial for people with Duchenne muscular dystrophy (DMD).
Benefits:
- Improved joint range of motion: The buoyancy of water reduces stress on joints, making it easier to move through a wider range of motion. This can help to improve flexibility and maintain muscle function.
- Maintained muscle strength: Hydrotherapy allows people with DMD to perform exercises that would be difficult or impossible on land due to the support provided by the water. This can help to maintain muscle strength and slow the progression of the disease.
- Improved cardiovascular health: Hydrotherapy can be a good form of exercise for people with DMD, as it can help to improve cardiovascular health.
- Pain relief: The warmth of the water can help to relieve pain and muscle stiffness.
- Psychological benefits: Hydrotherapy can be a fun and enjoyable activity for people with DMD. It can also provide a sense of social interaction and support.
Stretching:
Duchenne muscular dystrophy (DMD) is a genetic condition that causes progressive muscle weakness. Stretching is an important part of managing DMD because it can help to:
- Maintain flexibility in the joints
- Prevent contractures (tightening of muscles and tendons)
- Improve range of motion
- Reduce pain
Additional Tips:
Important things to keep in mind:
- It’s important to consult with a physical therapist to develop a personalized stretching program that is safe and effective for you or your child.
- Stretches should be done slowly and gently. Bouncing or forcing a stretch can cause injury.
- Each stretch should be held for 30-40 seconds and repeated 2-4 times.
- Stretching should be done regularly, ideally every day or every other day.
Low-resistance stationary cycling:
Low-resistance stationary cycling can be a beneficial form of exercise for people with Duchenne muscular dystrophy (DMD). DMD is a progressive muscle weakness condition, and exercise is an important part of managing the symptoms and maintaining strength for as long as possible.
Benefits:
Benefits of low-resistance stationary cycling for DMD:
- Improves cardiovascular health
- Maintains muscle strength and function
- Increases flexibility
- Improves range of motion
- Helps to maintain bone density
- Reduces fatigue
- Improves mood and well-being
Important considerations:
- It is important to start with low resistance and gradually increase it as tolerated.
- It is also important to listen to your body and take breaks when needed.
- A physical therapist can help you develop a safe and effective exercise program.
Types of stationary cycles for DMD:
There are a variety of stationary cycles available, including upright bikes, recumbent bikes, and handcycles. The best type of bike for someone with DMD will depend on their individual needs and abilities.
- Upright bikes: These are the most common type of stationary bike. They can be a good option for people with DMD who have good upper body strength and balance.
- Recumbent bikes: These bikes have a reclining seat, which can be more comfortable for people with DMD who have difficulty sitting upright.
- Handcycles: These bikes are powered by the arms instead of the legs. They are a good option for people with DMD who have leg weakness.
Aquatic therapy:
Aquatic therapy, also known as hydrotherapy, is a form of physical therapy that takes place in a warm water pool. It can be a beneficial treatment for people with Duchenne muscular dystrophy (DMD), a genetic condition that causes progressive muscle weakness.
Benefits:
- Improved range of motion: The buoyancy of water can help to support the body and reduce stress on the joints, which can make it easier to move through a wider range of motion. This can help to improve flexibility and prevent contractures.
- Increased muscle strength: Aquatic therapy can help to maintain or even improve muscle strength. The resistance of water can provide a challenging workout, and the buoyancy can help to protect the muscles from injury.
- Improved cardiovascular health: Aquatic therapy can be a good way to get exercise without putting too much stress on the heart. This can be important for people with DMD, who may have weakened heart muscles.
- Pain relief: The warmth and buoyancy of water can help to relieve pain and stiffness.
- Improved balance and coordination: Aquatic therapy can help to improve balance and coordination, which can help to reduce the risk of falls.
- Psychological benefits: Aquatic therapy can be a fun and enjoyable activity, which can improve mood and quality of life.
Techniques:
Aquatic therapy sessions typically last for 30 to 60 minutes. The therapist may use a variety of techniques, such as:
- Range-of-motion exercises
- Strengthening exercises
- Aerobic exercises
- Balance and coordination exercises
- Safety precautions
Aquatic therapy is generally safe for people with DMD. However, it is important to take some safety precautions:
- Always warm up before starting any exercises.
- Cool down after your workout.
- Be aware of your surroundings and avoid slipping or falling.
- Let your therapist know if you experience any pain or discomfort.
Electrical stimulation:
Electrical stimulation (NMES) is a technique that uses electrical pulses to cause muscle contractions. It is being investigated as a potential treatment for Duchenne muscular dystrophy (DMD), a genetic disorder that causes progressive muscle weakness.
Studies in animal models of DMD have shown that NMES can improve muscle strength, function, and survival. For example, a study published in e Life found that zebrafish with DMD who were treated with NMES had improved muscle structure, function, and swimming ability.
However, the research on the use of NMES in humans with DMD is limited. Some small studies have shown that NMES can improve muscle strength in the legs, but other studies have found no benefit. More research is needed to determine whether NMES is a safe and effective treatment for DMD.
Important points to consider:
- NMES is not a cure for DMD, but it may be a helpful tool for managing the symptoms of the disease.
- NMES should only be used under the supervision of a healthcare professional.
- NMES is not right for everyone with DMD. People with certain medical conditions, such as pacemakers or implanted defibrillators, may not be able to use NMES.
What are preventive measures for Duchene muscular dystrophy?
Preventive measures:
Preventive measures for Duchenne muscular dystrophy (DMD) primarily involve genetic counseling and early detection:
- Genetic Counseling: If there is a family history of DMD, consider genetic counseling to assess the risk of passing on the gene mutation to future children.
- Prenatal Testing: For families at risk, prenatal genetic testing can identify the presence of the DMD gene mutation in a developing fetus.
- Carrier Testing: Women with a family history should consider carrier testing to determine if they carry the DMD gene mutation.
- Early Diagnosis: Promptly seek medical evaluation if you suspect DMD in a child. Early diagnosis can lead to better management and interventions.
- Physical Therapy: Physical therapy and exercise can help maintain muscle function and mobility in individuals with DMD.
- Medications: Consult with a healthcare professional for medications like corticosteroids, which may help slow the progression of DMD symptoms.
- Supportive Care: Provide emotional and psychological support to individuals and families affected by DMD.
Conclusion:
In conclusion, Duchenne muscular dystrophy is a complex genetic disorder that requires a multidisciplinary approach to management. Physical therapy, along with other interventions, plays a vital role in optimizing function, mobility, and overall well-being for individuals with DMD. Continued research and advancements in treatment hold promise for improving outcomes and ultimately finding a cure for this debilitating condition.
FAQ’s :
How does Physical therapy help Duchenne muscular dystrophy (DMD)?
Duchenne muscular dystrophy (DMD) is a genetic disorder that causes progressive muscle weakness. Physical therapy can’t cure DMD, but it can play an important role in managing the condition and improving quality of life for people with DMD.
Here are some of the ways physical therapy can help people with DMD:
- Maintain muscle strength and function: Physical therapists can teach people with DMD exercises to help them maintain muscle strength and function for as long as possible. This can include exercises to improve range of motion, flexibility, and balance.
- Prevent contractures: Contractures are a common complication of DMD. They occur when muscles become shortened and tight, making it difficult to move joints. Physical therapists can help to prevent contractures by stretching muscles and teaching people with DMD how to stretch at home.
- Improve gait and posture: Physical therapists can help people with DMD to improve their gait (walking pattern) and posture. This can help to reduce pain and fatigue, and make it easier to get around.
- Manage pain: Physical therapists can teach people with DMD techniques to manage pain, such as massage, heat therapy, and cold therapy.
- Increase independence: Physical therapists can help people with DMD to learn how to use assistive devices, such as wheelchairs and braces. This can help them to stay independent and participate in activities of daily living.
What happens to DMD muscles during exercise?
Duchenne muscular dystrophy (DMD) is a genetic condition that causes progressive muscle weakness. It affects a protein called dystrophin, which is essential for keeping muscle cells healthy. In people with DMD, the lack of dystrophin makes their muscles more susceptible to damage during exercise.
There are two main concerns with exercise and DMD:
- Muscle damage: Exercise can cause tears in the muscle fibers of people with DMD. This damage can worsen muscle weakness and lead to pain and inflammation.
- Inefficient exercise: Because of the lack of dystrophin, DMD muscles may not be able to efficiently use energy during exercise. This can lead to fatigue and make it difficult to sustain activity.
However, research suggests that carefully regulated exercise programs can have some benefits for people with DMD, such as:
- Improved muscle strength and endurance
- Reduced muscle loss
- Delayed progression of muscle weakness
- Improved cardiovascular health
- Increased bone density
- Improved mental and emotional well-being
What muscles are weak in DMD?
Duchenne muscular dystrophy (DMD) is a genetic disorder that causes progressive muscle weakness. The weakness typically starts in the legs and pelvis, and then spreads to the arms, shoulders, and trunk.
Here’s a breakdown of the muscle weakness progression in DMD:
- Early stages (ages 3-5):Weakness affects the shoulder and upper arm muscles, along with the muscles in the hips and thighs. This can lead to difficulty with tasks like running, jumping, climbing stairs, and getting up from the floor.
- Later stages (teenage years):Muscle weakness spreads to affect the lower legs, forearms, neck, and trunk. The calves may appear enlarged due to fat and connective tissue replacing muscle (pseudohypertrophy). As the disease progresses, the breathing muscles may also weaken, leading to respiratory problems.
- Advanced stages (adulthood): In severe cases, weakness can affect all muscles, including those needed for breathing and swallowing. People with DMD may require assistance with daily activities and use a wheelchair to get around.
I am a highly skilled and experienced content writer with a Doctorate in Therapy degree. With a deep understanding of the human body and a passion for health and wellness. I combines my clinical expertise and writing skills to create valuable and engaging content.