Pelvic pain is a common yet complex condition that can affect both men and women. It can be acute or chronic and may originate from various systems in the body, including the reproductive, urinary, gastrointestinal, or musculoskeletal systems. This article explores the potential causes, symptoms, and treatment options for pelvic pain.
what is pelvic pain?
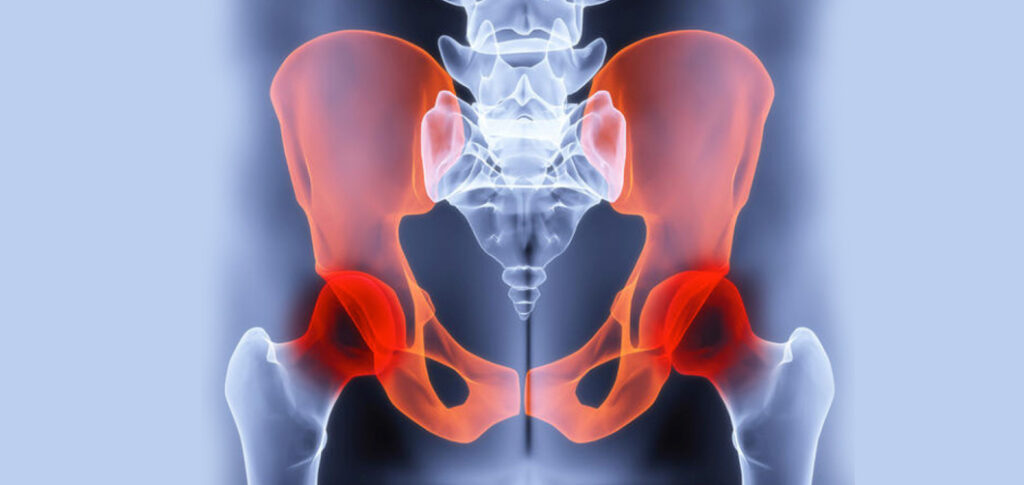
Pelvic Pain
Pelvic pain is a common issue that can affect both men and women. It’s felt in the lower abdomen, below the belly button and extending towards the groin. The pain can vary from sharp and stabbing to dull and achy. While it’s often a cause for concern, pelvic pain can arise from many reasons, some serious and others not.
What are common types of pelvic pain?
Types:
Pelvic pain can be a general term for discomfort or pain in the lower abdomen, below the belly button and above the thighs. It can affect both men and women, though it’s more common in women. There are many causes of pelvic pain, some more serious than others. Here are some of the most common types of pelvic pain:
- Endometriosis: This is a condition where tissue similar to the lining of the uterus (endometrium) grows outside of the uterus. This tissue can cause pain, especially during menstruation.
- Pelvic inflammatory disease (PID): This is an infection of the female reproductive organs. It can cause pelvic pain, as well as other symptoms such as fever, vaginal discharge, and pain during urination or sexual intercourse.
- Ovarian cysts: These are sacs filled with fluid that can form on the ovaries. Most ovarian cysts are harmless, but some can cause pain, especially if they rupture or bleed.
- Urinary tract infections (UTIs): These are infections of the urinary system, which includes the kidneys, ureters, bladder, and urethra. UTIs can cause pelvic pain, as well as burning with urination, frequent urination, and blood in the urine.
- Interstitial cystitis (IC): This is a chronic condition that causes inflammation of the bladder wall. It can cause pelvic pain, as well as frequent urination, urgency to urinate, and pain during urination.
- Muscle strain: The muscles in the pelvis can be strained from overuse, injury, or childbirth. This can cause pelvic pain, especially during certain activities such as exercise or sexual intercourse.
What are different Causes of pelvic pain?
Causes:
- Reproductive Issues (Women): Conditions like menstrual cramps, ovulation, endometriosis, uterine fibroids, and pelvic inflammatory disease (PID) can all cause pelvic pain.
- Urinary Tract Issues: Urinary tract infections (UTIs) and bladder problems can irritate the bladder and cause pelvic pain.
- Digestive Issues: Constipation, irritable bowel syndrome (IBS), and diverticulitis can cause pain in the pelvic region.
- Muscle Strain: Straining the muscles in your pelvis during exercise or heavy lifting can lead to pain.
- Endometriosis: Tissue similar to the uterine lining grows outside the uterus, causing inflammation and pain.
- Sexually Transmitted Infections (STIs): STIs like chlamydia and gonorrhea can cause pelvic pain, especially in women.
- Other Causes: Appendicitis, kidney stones, and even psychological factors like stress can contribute to pelvic pain.
What kind of symptoms present in pelvic pain patient?
Symptoms:
- Aching or sharp pain in the lower abdomen or lower back
- Pain during urination or sexual intercourse
- Pain that worsens during menstruation
- Unusual vaginal discharge
- Bleeding between periods
Differential diagnosis:
Pelvic pain is a common symptom experienced by many people. It can be caused by a variety of factors, ranging from gynecological conditions to musculoskeletal problems. Because of this, diagnosing the cause of pelvic pain can be challenging. Here’s a breakdown of the different categories a doctor might consider when diagnosing pelvic pain:
Gynecological Causes:
- Endometriosis: This condition occurs when tissue similar to the lining of the uterus (endometrium) grows outside the uterus. Endometriosis can cause pelvic pain, especially during menstruation.
- Pelvic inflammatory disease (PID): An infection of the reproductive organs. PID can cause pelvic pain, as well as abnormal vaginal discharge and pain during sex.
- Ovarian cysts: Sacs filled with fluid that can form on the ovaries. Most ovarian cysts are harmless, but some can cause pelvic pain, especially if they rupture or bleed.
- Uterine fibroids: Noncancerous tumors of the uterus. Fibroids can cause pelvic pain, as well as heavy bleeding and pressure on the bladder or bowels.
Musculoskeletal Causes:
- Muscle strain or spasm: The muscles in the pelvis can become strained or spastic, which can cause pelvic pain.
- Endometriosis: Though listed above in gynecological causes, endometriosis can also irritate nerves and muscles in the pelvis, leading to pain.
- Irritable bowel syndrome (IBS): A digestive disorder that can cause cramping, bloating, and diarrhea. IBS can sometimes mimic pelvic pain.
Other Causes:
- Appendicitis: Inflammation of the appendix. Appendicitis can cause severe pain in the lower right abdomen, which can sometimes be mistaken for pelvic pain.
- Kidney stones: Stones can cause sharp pain in the lower abdomen or back.
- Urinary tract infection (UTI): An infection of the urinary system. UTIs can cause pelvic pain, as well as burning with urination and frequent urination.
Additional Tips:
Here are some additional things to keep in mind:
- Pelvic pain can be acute (sudden and severe) or chronic (lasting for more than 6 months).
- The character of the pain can also vary, from sharp and stabbing to dull and achy.
- Pelvic pain may be worse during certain times of the menstrual cycle or during sexual intercourse.
What are Treatment option for pelvic pain?
Treatment:
Treatment for pelvic pain depends on the underlying cause. It can involve:
Medications:
Pelvic pain can arise from various causes, including gynecological conditions, urinary tract issues, gastrointestinal problems, and musculoskeletal disorders. The choice of medication depends on the underlying cause. Here are some commonly used medications for managing pelvic pain:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These include ibuprofen (Advil, Motrin) and naproxen (Aleve). They help reduce inflammation and alleviate pain.
- Acetaminophen: Commonly known as Tylenol, acetaminophen can help relieve pain without reducing inflammation.
- Hormonal Treatments: Birth control pills, patches, or rings may help manage pain related to menstrual cycles, endometriosis, or other hormonal imbalances.
- Antibiotics: If the pelvic pain is due to an infection, such as a urinary tract infection (UTI) or pelvic inflammatory disease (PID), antibiotics may be prescribed.
- Antidepressants: Tricyclic antidepressants (e.g., amitriptyline) and selective serotonin reuptake inhibitors (SSRIs) can help manage chronic pain conditions, including pelvic pain.
- Anticonvulsants: Medications like gabapentin (Neurontin) or pregabalin (Lyrica) are sometimes used for nerve-related pain.
- Muscle Relaxants: For pain related to muscle spasms, muscle relaxants such as cyclobenzaprine may be prescribed.
- Opioids: In severe cases, opioids may be used for pain relief. However, these are generally considered a last resort due to their potential for addiction and side effects.
- Topical Treatments: Lidocaine patches or gels can provide localized pain relief.
- Gastrointestinal Medications: For pain related to gastrointestinal issues, antispasmodics or medications for irritable bowel syndrome (IBS) may be used.
It’s essential to consult a healthcare provider for a proper diagnosis and treatment plan tailored to the specific cause of pelvic pain. They can provide guidance on the most appropriate medication.
Physical Therapy:
Pelvic floor physical therapy is a type of physical therapy that can help relieve pelvic pain. Pelvic pain is pain felt in the lower abdomen (stomach area), pelvis, or perineum (the area between the rectum and the scrotum or vagina). It can be caused by a variety of factors, including:
- Muscle tightness or weakness
- Endometriosis
- Interstitial cystitis
- Pelvic inflammatory disease (PID)
- Nerve pain
- Past surgeries or childbirth
Pelvic floor physical therapists are specially trained to assess and treat the pelvic floor muscles. These muscles support the bladder, uterus (in women), and rectum. When the pelvic floor muscles are weak or tight, they can cause pain.
How it works:
A pelvic floor physical therapist will work with you to develop a treatment plan that may include:
- Exercises to strengthen or relax the pelvic floor muscles
- Manual therapy to improve flexibility and circulation
- Biofeedback to help you learn to control your pelvic floor muscles
- Electrical stimulation to help reduce pain and muscle spasms
Pelvic floor physical therapy can be a very effective treatment for pelvic pain. If you are experiencing pelvic pain, see a doctor to rule out any underlying medical conditions. If your doctor determines that pelvic floor physical therapy is right for you, they can refer you to a qualified therapist.
Benefits:
Here are some of the benefits of pelvic floor physical therapy:
- Reduced pain
- Improved bladder control
- Improved bowel control
- Improved sexual function
- Improved quality of life
Surgery:
Surgery is one of the treatment options for pelvic pain, but it’s usually considered after other nonsurgical treatments have been tried. There are different types of surgery for pelvic pain, depending on the underlying cause.
- Laparoscopyis a minimally invasive surgery that uses a small camera inserted through an incision in the abdomen to view the pelvic organs. This surgery can be used to diagnose and treat endometriosis, pelvic adhesions, and ovarian cysts.
- Hysterectomy is the surgical removal of the uterus. It may also involve the removal of the ovaries and fallopian tubes. A hysterectomy is a majorsurgery and is usually only considered as a last resort for pelvic pain.
- Myomectomyis the surgical removal of uterine fibroids. Fibroids are benign tumors that grow on the wall of the uterus. Myomectomy can be performed laparoscopically, vaginally, or abdominally.
Additional Tips:
Here are some things to keep in mind if you are considering surgery for pelvic pain:
- Surgery is not always a cure for pelvic pain.
- There are risks associated with any surgery, such as infection, bleeding, and anesthesia complications.
- Recovery from surgery can take time.
You should discuss all of these factors with your doctor before making a decision about surgery.
Lifestyle Changes:
Pelvic pain can be really disruptive, but there are some lifestyle changes that can help manage it. Maintaining a healthy weight, managing stress, and practicing good posture can all help alleviate pelvic pain. Here are some things you can consider:
- Exercise: Regular, low-impact exercise like walking or swimming can improve your mood, reduce stress, and even help regulate hormones that may be contributing to pain.
- Diet: Maintaining a healthy weight can take pressure off your pelvic floor. You might also want to consider if certain foods trigger your pain and keep a food diary to track this.
- Sleep: Getting enough quality sleep is important for overall health, but also for managing pain. Make sure you have a relaxing bedtime routine and prioritize good sleep hygiene.
- Stress management: Chronic stress can worsen pelvic pain. Techniques like meditation, yoga, or deep breathing can help you relax and manage stress levels.
Additionally:
- Pelvic floor muscle exercises: A physical therapist can teach you Kegel exercises to strengthen your pelvic floor muscles, which can improve symptoms.
- Good posture: Sitting and standing with good posture can help reduce strain on your pelvic floor.
What kind of exercises are important for pelvic floor muscles?
Kegel exercises:
Pelvic floor muscle exercises, also known as Kegel exercises, can strengthen the muscles that support your bladder, uterus (in women), and rectum. Strong pelvic floor muscles can help with various issues including incontinence, sexual function, and pelvic organ prolapse.
Guidelines:
Here’s a basic guide to get you started with Kegel exercises:
- Finding the muscles: Imagine you’re trying to stop yourself from urinating midstream. The muscles you clench to do that are your pelvic floor muscles. You can also try lying on your back with your knees bent and feet flat on the floor. Tighten your abdominal muscles and squeeze the muscles around your urethra and vagina (if you have one) as if you’re trying to hold in gas.
- The squeeze: Once you’ve identified the muscles, tighten them gently and hold for a count of 3-5 seconds. Focus on tightening the pelvic floor muscles, not your buttocks or abdominal muscles.
- Relaxation: Relax your pelvic floor muscles completely. This is just as important as the squeeze.
- Repetitions and sets: Aim for 3 sets of 10 repetitions daily. You can do these exercises in any position – lying down, sitting, or even standing.
- Progression: As you get stronger, you can gradually increase the duration of the squeeze and relaxation phases.
Additional Tips:
Here are some additional tips:
- Breathe normally throughout the exercise.
- Don’t strain or push yourself too hard.
- Be consistent with your exercises. It may take a few weeks to see results
Variations :
There are a few variations of Kegel exercises you can try to target different parts of your pelvic floor muscles:
- Basic Squeeze: This is the most common Kegel exercise. Imagine you’re trying to stop the flow of urine midstream. Tighten your pelvic floor muscles as if you’re doing this, hold for a few seconds, then relax.
- Short Pulses: Instead of holding the squeeze, try contracting and relaxing your pelvic floor muscles rapidly in short pulses.
- Long Holds: Once you’ve mastered the basic squeeze, extend the hold time to strengthen your muscles further. Aim for holding the squeeze for 5-10 seconds before relaxing.
- Inner Lift: Imagine you’re drawing your pelvic floor muscles up and inwards towards your navel. You can combine this with the basic squeeze for a more targeted exercise.
Conclusion:
Pelvic pain can significantly impact an individual’s quality of life, but with proper diagnosis and treatment, many people can find relief from their symptoms. It’s essential to consult with a healthcare professional to determine the underlying cause of pelvic pain and develop an appropriate management plan tailored to individual needs. By addressing the physical, emotional, and psychological aspects of pelvic pain, individuals can regain control and lead fulfilling lives.
FAQ’s:
What causes female pelvic pain?
Female pelvic pain can arise from a variety of reasons, affecting the reproductive organs, urinary system, digestive system, muscles and ligaments, or nerves in the pelvis.
Here are some possible causes of female pelvic pain:
Reproductive system issues:
- Endometriosis: tissue similar to the uterine lining that grows outside the uterus
- Pelvic inflammatory disease (PID): an infection of the female reproductive organs [Pelvic inflammatory disease]
Ovarian cysts or tumors
- Uterine fibroids: noncancerous tumors in the uterus
- Vulvodynia: chronic vulvar pain
- Cervical cancer, ovarian cancer, or uterine cancer
Urinary system issues:
- Urinary tract infections (UTIs)
- Bladder stones
Digestive system issues:
- Irritable bowel syndrome (IBS)
- Constipation
- Diverticulitis: inflammation of the pouches in the lining of the colon
Musculoskeletal issues:
- Tightness or spasm of pelvic floor muscles
- Endometriosis
- Pelvic organ prolapse: when the pelvic organs drop down from their usual position
Nerve issues:
- Sciatica: pain that radiates from the lower back down the leg
- Meralgia paresthetica: a tingling or burning sensation in the outer thigh
Other causes:
- Appendicitis
- Pregnancy complications, such as ectopic pregnancy or miscarriage
Is walking good for pelvic pain?
Walking can be good for pelvic pain in many cases. Here’s why:
- Strengthens pelvic floor: Walking engages the pelvic floor muscles, which can help improve their strength and tone. Stronger pelvic floor muscles can better support the pelvic organs and reduce pain.
- Low impact: Walking is a low-impact exercise that puts minimal stress on the joints, unlike activities like running or jumping. This can be beneficial if your pelvic pain is related to musculoskeletal issues.
Important tips:
However, it’s important to consider some things:
- Severity of pain: If walking worsens your pain, it’s best to rest or try a different activity.
- Cause of pain: Certain causes of pelvic pain might not respond well to walking.
Here are some tips for walking with pelvic pain:
- Start slow: Begin with short walks and gradually increase the duration and intensity as tolerated.
- Listen to your body: If you experience pain, stop walking and rest.
- Proper form: Maintain good posture while walking to avoid putting extra strain on your pelvis.
- Supportive shoes: Wear comfortable, well-fitting shoes with good arch support.
How is pelvic pain felt?
Pelvic pain can be felt in a variety of ways, including:
- A dull ache
- A sharp pain
- Throbbing pain
- Burning pain
- Pressure or cramping
The pain may be constant or come and go. It may also worsen with certain activities, such as sexual intercourse, exercise, or bowel movements.
Some people also experience pain in other areas along with pelvic pain, such as the lower back, abdomen, or thighs.
I am a highly skilled and experienced content writer with a Doctorate in Therapy degree. With a deep understanding of the human body and a passion for health and wellness. I combines my clinical expertise and writing skills to create valuable and engaging content.


A motivatting discussion is worth comment.
I think tht you need to publish more about
this topic, it might not be a taboo matter but generally folks don’t
speak about these topics. To the next! Best wishes!! https://www.waste-ndc.pro/community/profile/tressa79906983/